I have (mostly, uncomfortably, incredibly anxiously) decided to get an abdominoplasty early next year.
I can’t believe I am writing this, nevertheless committing to even considering it. It feels heavy, embarrassing, complicated and overwhelming to share, but it’s important for me, and maybe for you.
Before you read the last chapters of a long, long process, I need you to know the steps that have proceeded the topic of an abdominoplasty (also commonly referred to as a “tummy tuck”), especially because I have a different story than many of the ones we hear about.
There’s a stigma that is attached to this particular procedure, in my circle it’s “failure” to rehab a diastasis (did you try __? do this instead!). Other stigmas attached are vanity- not embracing your #mombod as is, being a quick fix for fat loss, becoming fake looking, or perpetuating the idea that abdominoplasty surgery is the only way to fix DR.
None of these are true, but they are loudly proclaimed or assumed. It’s hard to stand up to the stigmas because a major surgery is not where I wanted to be, nevertheless, one that’s *technically* optional. I also know, and own, that I am not someone who “looks like they need a tummy tuck.” I am fairly lean, my stomach is mostly flat unless I’m bloated (which happens easily with diastasis) and I am strong. So why would I need/want one? Why can’t I just love my body as is? Well, I DO….which is why this is complicated.
To examine a lot of this, we need to rewind a bit so you understand the full scope of considerations not just for me, but for all women who may NEED OR CHOOSE to have this kind of (very common) procedure. Because where are we getting our info and guidance on this kind of procedure? Google and mommy bloggers? Hmmm…that sounds all too familiar.
Let me explain some of the backstory.

6 years ago I was newly pregnant with Cade, navigating my “fit pregnancy” and having no true understanding of how to approach this chapter in my athleticism. Messages of “listen to your body!” “Do what you’ve always done!” “You were made for this!” infiltrated and was what I relied on for guidance. When I say there was NO talk of diastasis recti or pelvic health in my “athlete/fit mom” circle, I mean, there was NOTHING. It was pure negligence to spotlight “pre and postnatal fitness” but only what fit the bias and examples of glorification of a healthy pregnancy.
Those extremes are absolutely what resonated because the other examples of a fit pregnancy simply encouraged walking and yoga and I was just not into that. There was no middle ground. So, naturally as an athlete and experienced coach with an invincible attitude, who “knew my body and trusted it.” I bought into the “train for birth, you were made for this” messaging and I gravitated toward the badass pregnant woman because it helped me hold on to an identity I was terrified of losing.
My training (among other controllable and uncontrollable factors) contributed to my significant diastasis (which went unknown and misguided for a long time). I had high-pressure strategies and tendencies, and no awareness of how to make adjustments to better manage my training, core/pelvic health and mindset during this chapter in my athleticism.
After a traumatic delivery (emergency C-section after a 30+ hour unmedicated labor), I used exercise to “reclaim” my process and fight off my struggles with anxiety and depression, desperate to feel normal again. It didn’t work, of course. It took a long time to realize the damage I had endured and work to heal in many, many ways.
Desperate to fix myself, I opted for an umbilical hernia repair, thinking that would be the answer to helping my abdomen feel whole again.
I did this at 1 year postpartum, knowing that I had diastasis, but NOT knowing that I should have rehabbed FIRST, and then proceed with surgery after having kids since I was otherwise asymptomatic from the hernia. I was confused and just didn’t now what was wrong with me. I did not have guidance by a Doctor, practitioner, coach or friend who understood these multiple considerations regarding DR, hernias, etc. I was lost and felt so alone with the changes my body had endured from the inside out. I thought, well maybe fixing this hernia will fix what’s wrong with my core.
You don’t know what you don’t know….and then when you know better, you do better,
By 2 years postpartum, I had learned new pressure management strategies, found helpful and trustworthy resources and adjusted my training. I was able to rehab my 8cm separation to about 2-3cm, even with the mesh hernia repair in place. Sharing this process is what started my business, especially the online component since I was getting countless emails of other pregnant or postpartum athletes saying “OMG me too! Help! What do I do? Why did no one tell me?!”
Suddenly I was no longer alone in these struggles, and I did not want these women to feel alone and misguided in a sea of mixed or harmful messaging for my peers- athletes.
Between Cade (5) and Chance (1), I grew and nurtured my other baby, my business, where I dedicated every ounce of my heart, time, brain and soul to creating content and education for athletes and then coaches, so that I could do my part in making sure no one was left to feel like I did during such an empowering yet vulnerable time in life. Since “birthing” my business and building Pregnancy and Postpartum Athleticism, thousands of women have been coached, women’s health and performance have been merged, and hundreds of coaches all over the world are guiding women in their community and online, advocating and collaborating with quality and intention. I love this effort, messaging and the pursuit of a passion that I get to call my business, and I am forever grateful for the humbling lessons that kicked my ass in the direction it needed to go.
I wasn’t sure I could have another baby.
The thought of enduring that process mentally and physically was terrifying. I had come so far and I did not want to go through those struggles again. However, in my heart, I knew taking the risk would be worth the Chance. And my 10lb baby Chance was born August 5th 2017 via gentle cesarian in the most beautiful, healing way I could have imagined. You can and should read about that here. I controlled the factors I could surrounding my training during pregnancy and my recovery process and surrendered to the rest. It was very, very successful, again, in the ways I could control.
This big baby was a lot of stress on my body, in particular my abdominal wall, despite the best of awareness, strategies, and adjustments made, he grew straight out into my diastasis (the path of least resistance, of course). My unique consideration was the mesh at the umbilicus. There was so much tension there, that the mesh held tightly (I mean, it IS mechanically engineered material), but this impacted the fascia and how the load of the baby was distributed in my belly and against the fascia. Imagine pinching a balloon at the center and thinking about what that tethering would do to the pressure distribution, then add more air. Ok, so that’s basically what happened with my 10lb baby on a 5’3 frame with pre-exisiting “vulnerable” fascia.

My abdominal wall took a hit…a big one.
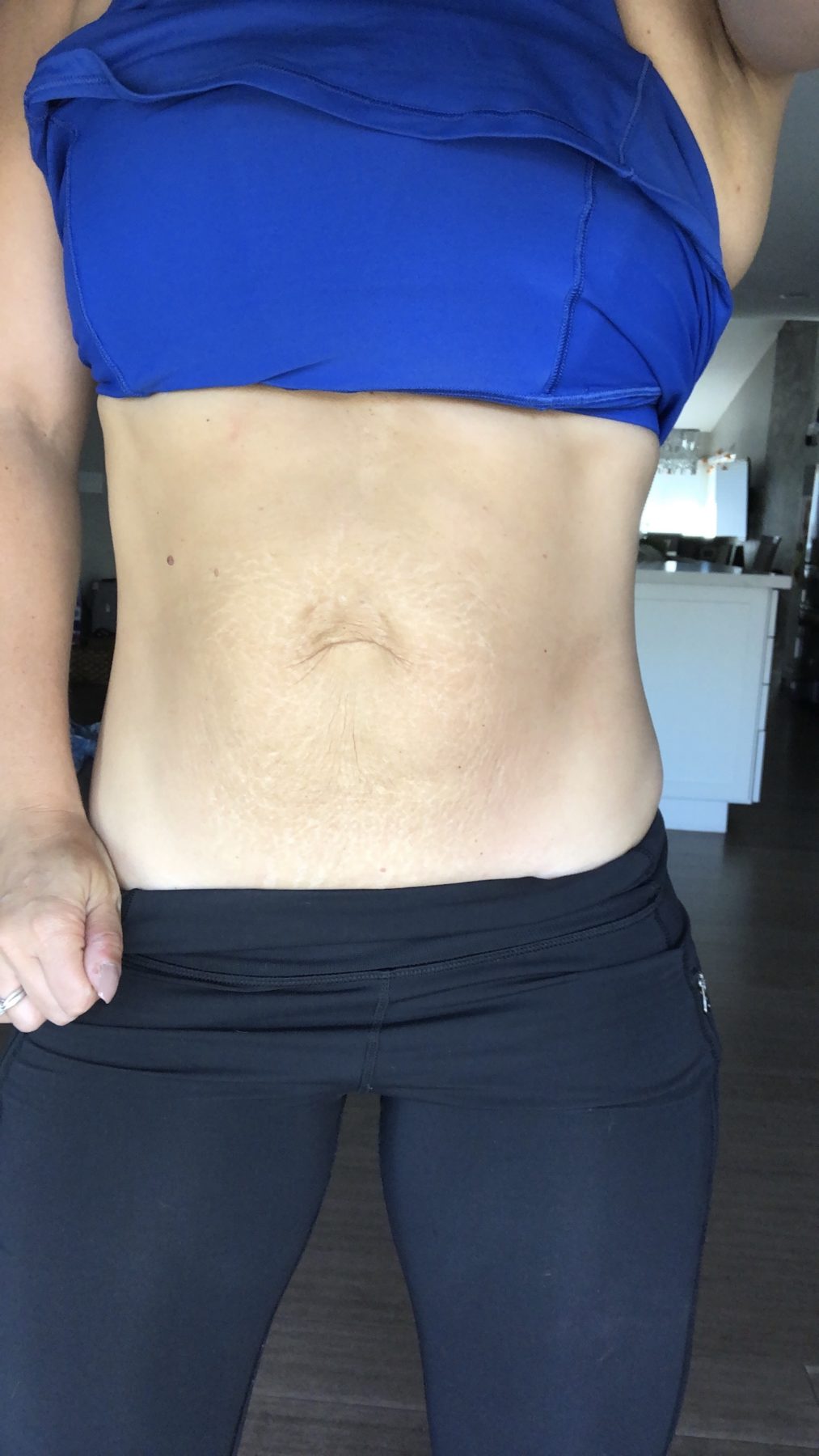
Unique considerations.
I did not fully know the “damage” to the fascia/rectus, particularly on the right side, until I was about 10 months postpartum when I could feel the edges of the rectus more. The left side has an edge, but the right side of my rectus where it meets the fascia of the Linea Alba feels frayed and the Linea Alba (line of the 6 pack abs) shifts diagonally to the right. I can approximate well with “exertion”- to about 2-3cm, but we don’t live at exertion and “pre-contraction.” This is why I am able to train and not feel too inhibited; I have strong strategies that know how to match the demand, and also, I’ve acclimated well to this body.
However, the edges of my rectus are flared, the mesh is damaged, there’s a new hernia and the fascia has simply taken a hit, in many ways, from high-pressure strategies, training, pregnancy x2, 2 big babies, 2 c sections, hernia repair, etc. This part of my body is technically injured, and I am managing the “injury” well, but there are factors out of my control at this point. It’s hard to know how to feel about this because I can defend surgery as much as I can defend not getting the surgery. I have tried really hard to take the emotion out of this, and look at my case objectively, just the facts of my patient profile, and from the analysis- I am a good candidate for this kind of procedure. But again, I feel easily swayed depending on the day. I am giving myself the space and time to keep processing this, but it’s important to share where I am at in this process currently.
This time around, I am fortunate to have some great resources for helping me navigate this chapter and all decisions; I’m anything but alone in this decision-making process. Antony Lo (Physiotherapist), Angela Spruill (Pelvic Floor Physical Therapist) and Haley Shevener (S&C coach/pre-postnatal trainer), have helped me walk through the variables of my case and have been affirming. However, even with trustworthy support, it still makes it hard with the immense amount of responsibility I feel to lead with intention, information and with a holistic approach.
I am expanding my spectrum of learning, healing, performance, and education both as a coach and athlete.
This is a huge learning curve, with uncharted territory involved.
This is what I do know and recommend…
- Adjust your training during pregnancy to understand how to manage your core and pelvic health for function and athleticism.
- Rehab postpartum with a Pelvic Floor Physical Therapist and qualified coach who can help progress and troubleshoot your individual needs.
- Give yourself TIME. And then even more time.

I have progressed to this without making my DR “worse.” My strategies support a variety of movement demands. - Ask questions. Ask more questions.
- 2cm and responsive fascia is considered “normal” and healed. If I did not have this mesh consideration, I *probably* would not opt for surgery because I have a “functional enough diastasis,” even with it being greater than 2cm, I can still function within my activities of daily living and training. We also believe the mesh is what’s preventing my fascia from being more responsive at the umbilicus area- my most vulnerable spot. We’ve always known this. It is why just doing a hernia repair is not the best option for me- it’s another hit to already vulnerable fascia and would be neglecting the greater consideration involved with a hernia and mesh- the structure in which it’s sitting on- a diastasis! Think of it like the foundation of a house- having that structural support is important for the longevity of it.
- Very few women need abdominoplasty surgery to repair diastasis recti. Rehab can work for the majority, with conservative care/progressive fitness regimen being the priority. I see it happen all the time! Expire rehab options FIRST, because understanding the pressure system will help heal if surgery is indicated.
- There will always be women who will need abdominoplasty surgery or CHOOSE to have it, because AUTONOMY. It’s ok to want to improve your appearance and function. Radical, I know. Do not perpetuate the stigma of shame for that choice or circumstance, especially if you coach or work with women.
- Find a surgeon who understands what you do, want to do and is willing to collaborate with your physical therapist and ideally a coach too, for prehab and rehab (I will be providing guidance on this down the line). I have been talking with Dr. Jamie Moenster, a Plastic Surgeon out of Tuscon, AZ for months now, and she has helped me explore multiple options as a friend and colleague. She is also an athlete who has treated me like a friend, welcoming me to get to know her, understand many options and logic through my best approach combining my expertise and hers. It’s been an incredible learning process so far. More on my process/game plan in part 2 of this blog series, where I’ll go over the approach of the actual procedure, which is slightly differently from “normal” abdominoplasty surgery.
- I wrote about the abdominoplasty surgery that I was fortunate to observe live (along with pictures) on this Instagram post. It’s fascinating and explains the step by step process for those who want the intricate details of how it works. I am so thankful Dr. Jamie and the patient allowed me to be present and involved.
There is a lot of help and ways to heal and abdominoplasty surgery can be (IS) one of them.
It hasn’t been talked about by many, myself included, but I will do my best to share openly, without fear of judgment and shame. I am scared but strategic, confident but conflicted, but most importantly, willing to show up and imperfectly practice brave with every step in this ongoing process. Stay tuned for part 2.



Thank you for writing this. I, too am struggling with the decision of whether to go forward with an abdominoplasty. Your thought processes are similar to my own and it was so nice to see it on paper! I struggle with the guilt of doing major surgery for “cosmetic” issues. I also struggle with the sacrifice of how much money it will cost. I have rehab my DR for so long. Again, thanks for your courage to share!
You’re awesome and the fact that you are open about this is great. Try not to be too embarrassed or shameful in telling everyone because most people who follow you take pride in their bodies and even the look. And there is nothing wrong with that! Body shaming happens body ways. So you do you and you’ll be happy you did this. It won’t be something you think about every day anymore and you can move on to bigger things in life 😊
Thanks so much for this!! Been dealing w DR for almost 8 years and while i have closed it considerably from 10 fingers and am pretty functional am finally considering surgery but am so afraid of recovery and financially. Looking forward to your journey.
Thank you so much for sharing this! You and Lisa Ryan are true pioneers. I am forever grateful for the both of you sharing your process and all the information for people like me.
Thank you so much for this post!! I have had four large babies and after my last, my doctor told me I needed this surgery because of my 8cm separation and hernias. I did not question it and went forward with the surgery. The missing piece to the puzzle was that I did not have any therapy before or after, so once I healed from the surgery I went back to lifting heavy and exercising but felt SO frustrated because I STILL had no idea how to use my stomach muscles – even with them sewn together. I have been following you for a while and am so thankful for your openness and help with navigating through all of this! Good luck with the surgery. The mental game I put myself through was the hardest to recover from. Try to push the guilt and embarrassment out of your mind. You’ve got this!!! Thanks again for all that you do!
Thank you so much for sharing this!! Like you I’m into fitness. I developed DR during my second pregnancy. Before getting pregnant I was in the best shape of my life. I continued to go to the gym and just kept doing what I always did as long as it felt good. Unfortunately, after the birth of my daughter I became aware that I was doing things that were most likely making my DR worse. Immediately after I had her I knew something was wrong with my core. I saw several doctors and they couldn’t explain my pain and many hadn’t even heard of Diastasis Recti. I researched and researched and came across a lot of information on blogs such as yours. There is a lot of information out there some I agree with and some I do not based on my experience. I armed myself with knowledge. I was going to beat DR and feel whole again. I longed to be able to lift heavy weights, to run again and workouts intensely. I made a plan. I completed MUTU System. I literally thought if I completed it my rectus muscles would be fused back together. I didn’t see an improvement so did it again. The second time around I hired a mutu pro trainer. I went to physiotherapy twice a week for about 5 months then would rotate back and forth from once to twice a week after that. I did the exercises given to me by my physiotherapist everyday sometimes twice a day. I took collagen, did acupuncture, Lazer therapy, the list goes on. Anything to heal my DR. I had never tried harder at anything. I found it so incredibly defeating when I was trying so hard and didn’t notice a difference. In fact I felt like my DR was getting worse. I had chronic low back pain, chronic pelvic and hip pain as well as digestive issues and chronic bloating. Finally I spoke with a couple of physiotherapists that had surgery. They both were incredibly happy with their results. Like me they wanted surgery mainly to restore function in their core. Even with their testimonies I still struggles with resorting to it. I felt like I was giving up in a sense. From what I was told it is rare to need surgery. In the end I let that go, I had to. I was doing what was best for me and my body. My DR was consuming me, I was feeling miserable mentally and physically almost all the time. Bottom line it was affecting my physical and mental heath and that was affecting my family life.
I had my DR surgically repaired just over a year ago. It has been life changing. I feel put back together. I no longer have pain and I now have a functional core. I’m doing everything I want to physically. I no longer feel held back. The old me is back! I wish I had seen a post like this when I was researching surgery. It would have been so helpful. Again thank you for being so open and brave. You are helping so many women!
I wish you all the best in your journey!
Thank you so so so much for this. You and I have exchanged messages about my case. After my twins were born I had a 15 cm DR and hernia. I had the hernia repaired with mesh twice and both failed and never knew that I should have seen a PFPT first so now I’m looking at the same thing. I’ve worked extensively with my PFPT to heal but can only do so much with this mesh. I understand how your feeling and I really appreciated your post on the surgery that you got to view. It took a bit of the unknown fear away for me. I’m here with you and I appreciate how open and vulnerable you’ve been with your experience.
Thank you so much for sharing. It’s so true, there simply is not enough information out there. May I ask what some of the negative effects of the surgery can be? I only know of the positives however am not aware of the long term effects of the surgery. Thank you brave lady!